7 & 8 Months Post-Op
I guess you could say that months 7 & 8 of recovering from my spinal fusion came in like the proverbial lion and out like a lamb.
I can remember the exact moment when something didn’t feel quite right. It was a Friday in early December. We’d picked the girls up at school and driven to Disney World. The 2.5-hour drive was uneventful. (Long car rides still aren’t the easiest on my back, but they’re certainly doable, especially if I’m the passenger.)

We were riding the ferry to the Magic Kingdom when I noticed a pain in my lower back. It wasn’t the chronic, dull ache that spans my entire lower back most of the time. This was a sharper pain, and it was only on one side.
I took Tylenol and pushed through – we were at Disney World, after all. I was okay that evening and the following morning. But by the afternoon, it was apparent that certain movements were going to cause pain – including any sort of stretching.
This was both frustrating and alarming, as stretching is essentially one-half of my post-op fitness regimen – I walk and I stretch. Walk. Stretch. Walk. Stretch. After surgery I was desperate to get back to yoga, so I’d incorporated (what I thought was) gentle yoga into my stretching.
But my body wasn’t having it – not anymore.
Stretching the Limits
During my 3 month post-op visit with my surgeon, I’d been told that there was no benefit in “pushing through the pain.” If something hurt, I needed to listen to my body and stop what I was doing. I took that advice to heart. So when my body told me to stop stretching, I stopped. I hated it, but I stopped.
Specifically, I stopped any kind of stretching that involved my whole body or a bend at the waist – downward-facing dog, for example, or any of the warrior poses. Even with modifications, the pressure on my back was intense. I could still stretch my calves and quads, as long as I stayed completely upright. My hamstrings were a little trickier to stretch without bending, but since they’re so tight to begin with even the tiniest stretch was effective.
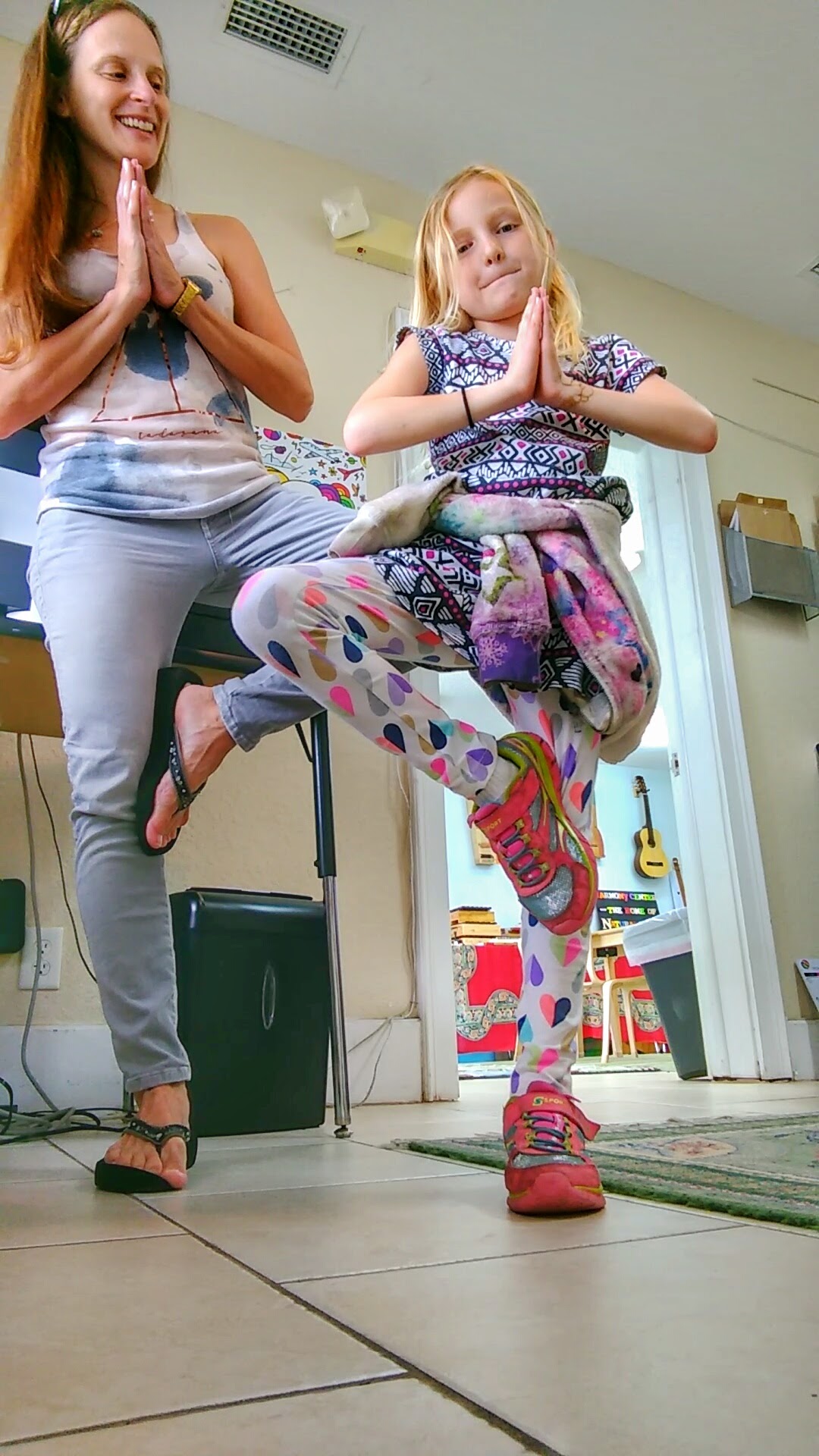
I sound kind of chipper about this, don’t I? Well, I wasn’t.
Avoiding most stretches helped me avoid acute pain, but in the meantime the ever-present ache in my lower back was getting worse. My whole body felt stiff. Had I caused the stiffness by not stretching, or had I prevented the stiffness and pain from getting worse? I didn’t know.
What I did know is that my activities of daily living were becoming more difficult, and my quality of life was declining. My BLT (bend, lift, twist) restrictions were lifted at 3 months, but I found myself unable to do any of the three without pain. I dreaded doing the laundry (even more than usual) because I had to squat down to put the clothes in & take them out of the dryer. And sneezing once again became the #1 most painful activity in an ordinary day, like it had been in my pre-fusion days.
I’ve shared that I felt as though the pace of my recovery slowed around 7 months, but a full-on regression? No way. I never would’ve guess that I’d feel better at 6 months post-op than I did at 8. I was disappointed, discouraged, and depressed.
Getting Worse, Not Better
After about 6 weeks of deteriorating health (both physical and mental), I finally called my surgeon. I shared my symptoms and concerns with him. From the info that I provided, he felt that it was unlikely that my pain was directly related to my surgery (e.g., a problem with my hardware or lack of bone growth). Rather, he suspected that the facet joint above or below my fusion (which is at L4-S1) had flared up.
He gave me 3 choices:
1. Have a CT scan with contrast. This would give the surgical team a clear picture of my surgery site and hardware, and it could conclusively determine if my current pain was directly resulting from my fusion. If a problem was present, we would explore further surgical options.
2. See my primary care physician to discuss non-surgical options. These would likely include anti-inflammatories, physical therapy, pain management, and epidural steroid injections – in other words, go through the same steps that I went through in 2015-2016 before deciding on surgery.
3. Do nothing.
I’d been “doing nothing” up to this point and it wasn’t working, so this wasn’t really a viable option for me. And the thought of going through all the treatment options again was disheartening. It felt like starting from scratch. The most appealing option was the CT scan – it would provide some definitive answers and would also let me take a peek at my back & hardware, which I haven’t done since my 3 month post-op appointment.
But here’s the catch with going the CT route (as I understood it). My surgical team is only allowed to treat me for surgical issues – past, present, or future. So if the CT scan showed that there was a problem directly related to my fusion (or indicating the need for additional surgical intervention), the next step would be to explore surgical options. But if the CT scan showed a nonsurgical issue (i.e., inflammation in a facet joint or a funky-looking disc), they wouldn’t be able to treat me at all.
(I know that’s a little confusing. Basically it means that I’m still considered a surgical patient, so my surgeon is able to do certain things like give me referrals or prescribe meds. If the issue wasn’t surgical, he wouldn’t be able to treat me.)
So even though I wanted the CT scan, my gut told me that it wasn’t necessary at this stage. My surgeon wasn’t concerned about the stability of my fusion or hardware. And I didn’t want to risk being discharged as a surgical patient. He offered to send me a referral to physical therapy and suggested that I follow up with my primary care doctor to formulate a treatment plan.
I wasn’t terribly happy with this but it was certainly the most palatable of the available options. In the meantime, since I had the doctor’s thumbs up, I started taking 800 mg of ibuprofen 1-2 x day. Ibuprofen had been my go-to medication in the months leading up to my surgery. It worked. Actually, it was the only thing that worked. Opioids (like hydrocodone or oxycodone) kind of take the edge off, and they knock me out so that the pain doesn’t bother me. But ibuprofen provides a bit of genuine relief for pain/discomfort related to inflammation. I had to stop taking it in the months before my fusion because I was starting to have terrible stomach pains. And after surgery, I was instructed to avoid all NSAIDs because they can inhibit healing and bone growth.
What I’m Doing Now
So I started taking ibuprofen, and I’ve been taking it regularly for about 3 weeks now. And guess what? I’m feeling significantly better. My surgeon was right. Something in my back was inflamed and causing me a whole lot of trouble. I still have back pain – I suspect that I always will, to some degree. But it’s no longer painful to stand up from a squat or bend to lift a (light) laundry basket. The acute pain is mostly gone.
I haven’t started physical therapy yet, and I’m not sure if I will. While I’m not opposed to PT, I think the real problem was that I was doing too much. I was pushing my body to do things that it wasn’t ready for. So here’s my current recovery regimen, prescribed by me:
1. Walking. Walking is the cornerstone of recovering from a spinal fusion and is recommended from (literally) day one.
The primary form of rehabilitation after spinal fusion is an aggressive walking program. You should start immediately after discharge, walking more and more each day. In general, we recommend two to three episodes of exercise per day. The average patient undergoing single-level surgery can be walking 15 minutes twice a day by their first postoperative visit and 30–40 minutes twice a day by six weeks after surgery. source
I love walking, but I have to fight the mindset that it is inferior to running.

2. Strengthening my core. A strong core will help stabilize my back. THESE are some of the exercises that I’m using. I’m also using THESE exercises to help strengthen my back muscles. The second article includes planks, but I find them much too hard on my back.
3. Gentle stretching. I mean really gentle. No arching, bending, twisting, or doing anything that feels even slightly bad. No amount of pain is good in this scenario.
4. No yoga. Or I should say almost no yoga. Breathing exercises are good, of course, as is meditation. I can do some very gentle hip openers and balance poses, but that’s about all. This one is the toughest on my ego, so some serious “suck it up, Buttercup” self-talk is required.

I also need to get plenty of rest, take my vitamins, drink lots of water, and stay cautious about bending/lifting/twisting. And I’ll continue to use the ibuprofen for a bit longer – hopefully I’ll get back on track and start making forward progress in my recovery again.
Much love, friends.
