In Part 1 of my Q+A, I talked about how I came to learn that I had spondylolisthesis. If you’re reading this because you’ve recently found out the same…I’m sorry. There’s no point in sugar-coating it – spondylolisthesis sucks.
Then again, if you’re reading this, you probably know that already.
Here’s the good news: the diagnosis itself doesn’t mean that your life is over, or even that it has to change dramatically. Surgery is not inevitable in all cases. The effects of spondylolisthesis can range from debilitating to barely noticeable. Hopefully you fall closer to the latter part of that range.
A number of factors will help your doctors categorize your spondy, which will help determine your treatment plan. Remember, though, that your surgeon/pain management specialist/x-ray technician isn’t inside your body. Medical tests don’t always tell the whole story. Ultimately, YOU will have to decide on (and in some cases, advocate for) the course of your treatment.
What Medical Tests Will I Have to Take? A number of tools can be used to diagnose and determine the severity of a spondy, including x-rays, MRIs, CT scans, myelogram, and bone scans. As I mentioned in my previous post, my spondylolisthesis was initially detected by a physical therapist and confirmed by MRI.
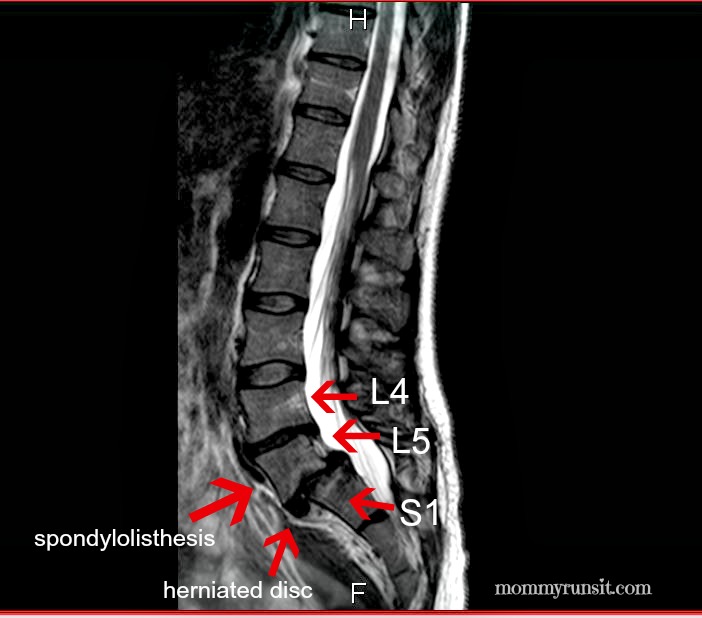
- Grade I – Less than 25% slip
- Grade II – Between 25 – 50% slip
- Grade III – Between 50 – 75% slip
- Grade IV – More than 75% slip
- Grade V – 100% slip, i.e. the upper vertebra has slid completely off the front of the lower vertebra. This is called spondyloptosis and is rare.
Stable vs. Unstable: A spondy slip can either be stable or unstable. With a stable slip, the vertebra has moved out of place but doesn’t appear to be slipping any further for the time being. An unstable slip shows movement of the vertebra when the person changes position (e.g., from laying to standing). An unstable slip is more vulnerable to a progression in the grade of the slip. A stable spondy is less likely, but certainly still at risk, for future movement.
The best way to determine the stability of a slip is with a series of four standing x-rays: (source)
- standing lateral (side view)
- standing oblique (taken at an angle from the back)
- flexion (bending forward)
- extension (bending backwards)
When reviewed side-by-side, these four x-rays can show the degree and amount of movement of a slip. Not all doctors will order these x-rays (mine didn’t). You may have to request them.
Nerve Damage and Other Symptoms
Spondylolithesis can range anywhere from asymptomatic to completely debilitating. Things start to get serious when the slipped vertebra is pressing on a spinal nerve root. (source) Symptoms include buttocks pain, leg pain or weakness, or numbness in the legs or feet. If the nerve root damage progresses, one might experience loss of bladder and/or bowel control. That indicates a very serious problem and requires immediate medical attention. If left untreated, all of these neurological complications have the potential to create permanent damage.
Your doctor should also discuss how your spondy impacts your life. How constant is your pain? Have you had to give up activities that you enjoy? Are you able to complete your activities of daily living unassisted?
From my understanding, the presence of nerve compression and damage are equally important as the grade and stability of a spondylolisthesis. Contrary to what you might think, a higher grade does not necessary equal more severe pain. I know people with Grade III spondys that are nearly asymptomatic and people with Grade I slips that cause constant and debilitating pain. So it’s all relative.
In my case, I had a Grade II spondylolisthesis (along with a Grade I retrolisthesis). This was determined solely by MRI. My surgeon did not order x-rays prior to surgery, and I’m not sure why – perhaps the grade of my slip along with my smushed discs at L4-L5 and L5-S1 were enough to warrant surgery? To be honest, I went into my neurosurgical consult thinking, “Well, he’s a surgeon, of course he’s going to recommend surgery.” But I’ve since learned that in other places and parts of the world, it’s common for doctors to refuse to perform spinal fusion for spondylolisthesis and related disorders.
My surgeon and I never discussed the stability of my slip. As a matter of fact, I learned about stable vs. unstable slips in a Facebook group AFTER my surgery. But as it turns out, my slip was unstable. The only reason I know this is because when my surgeon met with my husband after the procedure, Dr. W mentioned that there was more movement in my vertebrae than he’d expected. I didn’t even find this out until weeks after surgery, when my husband referenced it in an offhand remark. I lucked out – if left untreated, my unstable slip could’ve made my situation significantly worse.
The real problem with my spondy, though, was the nerve damage – specifically the persistent numbness in my right foot. Leg pain, tingling, and numbness in the legs and feet (or arms and hands for spondylolisthesis in the cervical spine) are red flags. I’ve heard that many surgeons will refuse to operate on people with ONLY back pain. This may be because a spinal fusion is effective in reducing leg pain, but back pain may persist even following a fusion. This is anecdotal though – I don’t know this for a fact, so don’t take my word for it!
What are the Conservative Treatment Options? Typically surgeons and/or insurance companies won’t consider surgical options until more conservative methods have been exhausted. These are the steps that I went through prior to my surgical consult. I know there are others – please feel free to add other treatment options in the comments.
1. NSAIDs (nonsteroidal anti-inflammatory drugs): I started out taking ibuprofen. Lots and lots of ibuprofen. And it actually provided me with some relief. The trouble is, ibuprofen has to be taken in high doses (400-800 mg) for it to have an anti-inflammatory effect. So I was taking 800 mg 2-3 times a day. Ibuprofen, especially at high doses, can irritate your stomach lining. So after a few weeks on this dose, I began to have very bad stomach cramps. I also tried a medication called Duexis, which combined ibuprofen with an antacid, but after a while these began to hurt my stomach too.
2. Oral and Injected Steroids: Corticosteroids can be used to suppress inflammation. I tried an oral taper pack and an injection (i.e., shot in the butt) of Solumedrol. Both provided mild but short-lived relief.
3. Physical Therapy: Initially, I had high hopes for physical therapy. Of course, that was back when I thought I was suffering from a running related injury and that physical therapy would be the solution, as it had been for a number of my runner friends. But once I learned more about my condition, I began to wonder how physical therapy could help me. My vertebrae were misaligned and compressing my nerves. All the core exercises in the world wouldn’t move my L5 back in place. Still, I insisted on continuing PT even after the therapist told me that I wasn’t a good candidate for it. I didn’t listen until I was “fired” by therapist #2 as well.
4. Epidural Steroid Injections: When meds and PT don’t do the trick, the next step is often to kick it up a notch. In my case, the “kick” came in the form of a steroid injection via epidural – i.e., medication injected directly into the problem area on my back. Like the other steroid treatments, the injections are supposed to reduce inflammation around the spinal nerves. In theory, reducing inflammation will alleviate the nerve compression, which will then provide some pain relief.
Some people find these injections helpful. I wasn’t one of them. I experienced a fairly uncommon complication during my first injection – I wound up in the ER with a post-dural puncture headache (i.e., a spinal headache) and required something called a blood patch to alleviate it. It was a miserable experience that by far overshadowed the little, if any, pain relief that I got from the epidural injection. (Please don’t let my experience scare you away. Just make sure you do your research. You can read more about epidural steroid injections HERE.)
My primary care physician and pain management doctor wanted me to continue receiving epidural injections, but one was plenty for me. Spinal headache aside, I just didn’t see how the injections were going to provide me with a long-term solution for my back and hip pain. Wouldn’t the pain come back as soon as the inflammation returned? And even if we managed to keep the inflammation under control, there was still that darned slipped vertebra to contend with. My primary doctor agreed and referred me to a neurosurgeon.
5. Surgical Consult: This is one of those situations where you should do as I say, not as I do. I’m embarrassed to admit that I went into surgery rather blindly. I chose my neurosurgeon because quite frankly, he’s the one my PCP referred me to – and I happened to like him. That’s also the only reason I chose a neurosurgeon over an orthopedic surgeon (both can perform a spinal fusion). I didn’t get a second opinion. I didn’t consider other non-surgical alternatives. I didn’t do enough research. I didn’t ask enough questions.
DON’T DO THIS.
At the very least, get a second opinion, maybe even a third. In my defense, I did make arrangements to get a second opinion from an orthopedic surgeon. But when I requested my medical records from the neurosurgeon, his nurse went to take me off the surgical schedule – I guess they didn’t want me taking up space if I was still undecided about surgery. At that point (March 2016), my surgery was scheduled two months out, which already seemed like a LONG time to wait. And when I found out that the process of getting a second opinion could potentially push me back another month or even longer, my husband and I decided that I should proceed with the May 2016 surgery date.
Was this the right decision? I’m not sure. I like my surgeon and so far I’m pleased with the results of my procedure, but I guess I’ll never know if a different doctor might have recommended an entirely different course of treatment.
To some extent, my lack of research was intentional – my fear was that it would only result in scaring me to death and maybe even second guessing my decision. Plus the internet is so full of horror stories – who knows what’s actually even true. I do wish that I’d found my online support group before surgery, because it has been a tremendous source of information and inspiration. (If you’re interested in joining, let me know in the comments and I’ll send you the info. It’s a private Facebook group.)
So. I decided to have surgery. I’ll tell you all about it next time.

p.s. In case you’re wondering how I’m doing at 3 months post-op, here you go: